
Introduction
Walk into most modern hospitals today and you’ll find something interesting: doctors staring at screens that seem to know more than they should. That’s not science fiction anymore. Artificial intelligence in healthcare has moved from research labs into actual patient care, and the shift happened faster than most of us realized.
The technology isn’t replacing doctors, despite what some headlines suggest. Instead, it’s becoming a tool that helps medical professionals catch things they might have missed, predict complications before they happen, and personalize treatments in ways that weren’t possible a decade ago.
For patients in the US and Pakistan alike, this means faster diagnoses, better accuracy, and sometimes the difference between catching a disease early or finding it too late.
What AI Actually Does in Medical Settings
The term “artificial intelligence” gets thrown around so much that it’s lost some meaning. In healthcare, we’re mostly talking about machine learning systems that analyze massive amounts of medical data and spot patterns that human eyes can’t catch.
Think of it this way: a radiologist might review thousands of X-rays in their career. An AI system can be trained on millions of images from around the world, learning to identify subtle signs of disease that even experienced doctors might overlook.
But here’s what matters more than the technology itself—how it’s actually being used right now.
Medical Imaging and Diagnostics
This is where AI has made the biggest splash, and for good reason. Detecting cancer, fractures, or internal bleeding from scans requires incredible attention to detail. Miss a small shadow on a lung X-ray, and a patient might not get treated until it’s much harder to cure.
AI diagnostic tools now assist radiologists by flagging suspicious areas on CT scans, MRIs, and mammograms. In some studies, these systems have matched or exceeded the accuracy of human specialists, particularly in detecting breast cancer and diabetic retinopathy.
Hospitals in major US cities have been using AI-powered imaging analysis for a few years now. The technology is starting to reach Pakistan as well, though access varies significantly between urban centers like Karachi and Lahore versus rural areas.
The real benefit isn’t that AI is “better” than doctors. It’s that it serves as a second pair of eyes, catching things that might be missed during a busy shift when a radiologist is reviewing their 50th scan of the day.

Predicting Patient Deterioration
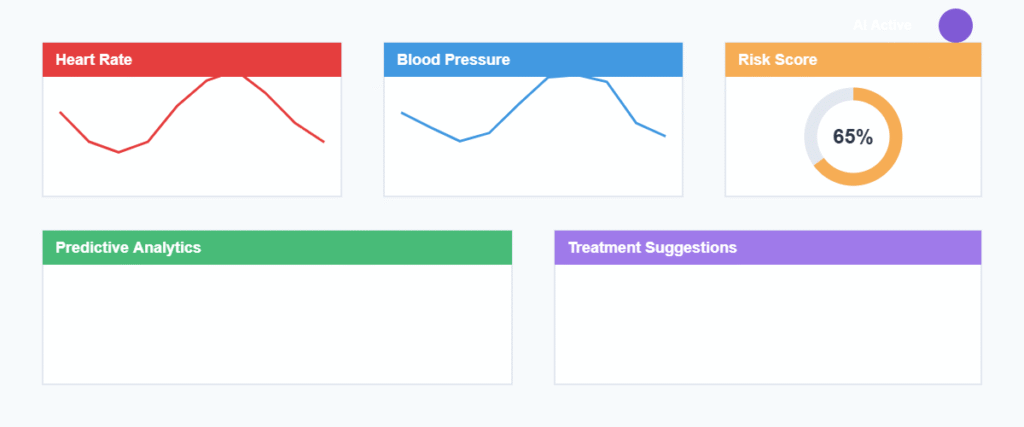
One of the more practical applications doesn’t get as much attention as it should. AI systems can now monitor patient vitals and predict which patients are likely to deteriorate in the next few hours.
This matters in intensive care units where early intervention can prevent cardiac arrest or septic shock. Instead of waiting for obvious warning signs, the system analyzes subtle changes in heart rate, blood pressure, and other metrics to alert nurses before a crisis develops.
Several hospital networks in the United States have reduced unexpected ICU transfers and mortality rates using these early warning systems. The technology relies on continuous data monitoring, which means it works best in well-equipped hospitals with electronic health records.
Drug Discovery and Development
Creating new medications typically takes over a decade and costs billions of dollars. AI is compressing some of that timeline by predicting which chemical compounds might work against specific diseases.
Pharmaceutical companies now use machine learning to simulate how thousands of molecules interact with target proteins, narrowing down which ones are worth testing in actual labs. This doesn’t eliminate the need for clinical trials, but it does cut years off the early research phase.
During the COVID-19 pandemic, AI helped identify existing drugs that might be repurposed for treatment. While not every prediction panned out, the speed at which researchers could test hypotheses was unprecedented.
Personalized Treatment Plans
Here’s where things get interesting for patients. Two people with the same diagnosis might respond very differently to the same treatment. AI systems can analyze a patient’s genetic information, medical history, and even lifestyle factors to recommend treatments that are more likely to work for that specific individual.
Oncologists are using this approach in cancer care, where AI helps determine which chemotherapy regimen or immunotherapy might be most effective based on the tumor’s genetic profile and the patient’s overall health.
This level of personalization was theoretically possible before, but the computational power required to analyze all that data in a reasonable timeframe simply wasn’t available. Now it is.
Challenges That Don’t Get Enough Discussion
The technology sounds impressive, and in many cases it is. But there are real problems that need addressing.
First, most AI systems are trained on data from Western populations, primarily from the US and Europe. This creates accuracy issues when the same systems are used in countries like Pakistan, where genetic diversity and disease patterns differ. A diagnostic AI trained mostly on Caucasian patients might miss important findings in South Asian populations.
Second, these systems are expensive. The hospitals that can afford cutting-edge AI tools are usually the ones in wealthy areas that already had good healthcare. This widens the gap between top-tier medical centers and smaller community hospitals.
Third, there’s the question of liability. When an AI system assists in a diagnosis and something goes wrong, who’s responsible? The doctor who followed its recommendation? The hospital that implemented it? The company that built the algorithm? Legal frameworks haven’t caught up with the technology yet.
The Doctor-Patient Relationship
Some worry that increasing AI use will make healthcare feel more impersonal. That’s a valid concern, but the reality seems more nuanced.
Doctors who use AI tools report that the technology actually gives them more time with patients because they spend less time on routine data analysis. Instead of manually reviewing every lab result looking for patterns, the AI flags what needs attention, and the doctor focuses on explaining options and listening to patient concerns.
The best implementations treat AI as a support tool, not a replacement. A patient doesn’t interact with the algorithm—they interact with their doctor, who happens to have access to better analytical tools.
What’s Coming Next
The current applications are just the beginning. Researchers are working on AI systems that can predict which patients are at risk for chronic diseases years before symptoms appear, allowing for preventive interventions that could save healthcare systems billions.
There’s also progress in using AI for surgical planning, where systems analyze previous successful surgeries to recommend optimal approaches for complex procedures. Some experimental systems even provide real-time guidance during surgery, though this remains controversial and largely experimental.
Mental health is another frontier. AI chatbots have shown promise in providing cognitive behavioral therapy for mild anxiety and depression, though they’re not replacements for human therapists in serious cases. The benefit is accessibility—people who can’t afford or access traditional therapy might benefit from AI-assisted mental health support.
Implementation in Developing Healthcare Systems
Pakistan’s healthcare system faces unique challenges that make AI both potentially transformative and difficult to implement. The country has a shortage of medical professionals, particularly in rural areas, which means AI diagnostic tools could help bridge some gaps in access to specialist care.
However, the infrastructure requirements are significant. AI systems need reliable electricity, internet connectivity, and integrated electronic health records—all of which remain inconsistent outside major cities.
Some Pakistani hospitals in Islamabad and Lahore have started piloting AI diagnostic tools, but widespread adoption will require investment in the underlying healthcare infrastructure, not just the technology itself.
Privacy and Data Security Concerns
Medical data is deeply personal, and AI systems require vast amounts of it to function effectively. This creates real privacy risks that patients should understand.
In the US, regulations like HIPAA provide some protection, but enforcement varies. In Pakistan, data protection laws are less developed, and patients often don’t know how their medical information is being used or stored.
Any hospital implementing AI should be transparent about what data is collected, how it’s used, and who has access to it. Patients deserve to know if their medical records are being used to train commercial AI systems, even if the data is supposedly anonymized.
The Cost Factor
Advanced AI healthcare tools aren’t cheap. A hospital might spend millions implementing these systems, costs that eventually get passed on to patients through higher bills.
In the US healthcare system, this adds to an already expensive landscape. In Pakistan, where out-of-pocket healthcare expenses already strain family budgets, the question becomes: who benefits from this technology?
The optimistic view is that AI will eventually reduce costs by catching diseases earlier and reducing unnecessary tests. The cynical view is that it becomes another profit center for hospitals and technology companies. The reality will probably fall somewhere in between.
Practical Advice for Patients
If your doctor mentions using AI as part of your diagnosis or treatment plan, asking a few questions is reasonable:
What specific role is the AI playing in your care? Is it analyzing images, predicting outcomes, or suggesting treatments?
What’s the accuracy rate of this particular system for your condition?
Is a human doctor reviewing the AI’s recommendations before making final decisions?
Most doctors will appreciate informed questions. If they get defensive about using AI tools, that might be a red flag.
The Reality Check
Artificial intelligence in healthcare is neither the miracle cure some claim nor the dystopian nightmare others fear. It’s a tool, and like any tool, its value depends on how it’s used.
The technology has already saved lives by catching cancers earlier, predicting patient deterioration, and personalizing treatments. It’s also created new challenges around access, privacy, and the growing gap between well-funded and under-resourced healthcare facilities.
For patients, the most important thing is understanding that AI is becoming part of the medical landscape whether we’re ready or not. The question isn’t whether to accept it, but how to ensure it’s implemented responsibly and benefits everyone, not just those who can afford premium healthcare.
The doctors making life-or-death decisions are still human. The algorithms are just helping them see a little more clearly. That’s progress worth acknowledging, even as we work through the very real problems that come with it.